You might not notice the small, nightly grind as you sleep, but that hidden habit can quietly strip enamel, cause cracks, and set the stage for tooth loss decades later. If you clench or grind in your 30s, you increase the risk of accelerated wear and damage that can lead to loose teeth and costly dental work down the road.
This article explains how bruxism develops in your 30s, how repeated pressure damages teeth and gums over time, and which long-term health risks untreated grinding can cause. You’ll also learn practical, proactive steps to protect your smile before minor wear becomes irreversible, especially if you are dealing with teeth grinding.
Table of Contents
ToggleUnderstanding Teeth Grinding in Your 30s
You may grind or clench your teeth because of stress, sleep disruption, medications, or bite issues. Early warning signs often show up as jaw pain, worn enamel, or morning headaches that, if ignored, increase risk of tooth fracture and loss.
Common Causes of Bruxism in Adults
Bruxism in your 30s often links to specific, identifiable triggers. Stress and anxiety increase jaw muscle tension and make nighttime clenching more likely.
Sleep disorders such as obstructive sleep apnea raise the chance of grinding by disrupting normal sleep cycles and activating bruxism episodes.
Certain medications — particularly some antidepressants and stimulants — can trigger or worsen teeth grinding for some people.
Bite problems and missing teeth change how your teeth contact each other, which can encourage habitual grinding as your jaw seeks a comfortable position.
Lifestyle factors matter too: heavy caffeine, alcohol use, and cigarette smoking all correlate with higher bruxism frequency.
Addressing the most relevant causes for you (stress management, sleep evaluation, medication review, dental alignment) reduces ongoing tooth wear.
Early Signs and Symptoms
You might notice morning jaw stiffness or a sore face when you wake up.
These symptoms signal that your jaw muscles are active at night and undergoing repeated strain.
Look for visible tooth changes: flattened, chipped, or shortened teeth and increased tooth sensitivity.
Enamel wear exposes dentin, making teeth more vulnerable to decay and fracture over time.
Headaches that begin at the temples, ear pain without an ear infection, and clicking or locking of the jaw joint (TMJ) are common.
If your partner reports audible grinding at night, treat that as a strong indicator that you need evaluation.
Prevalence Among Adults Aged 30-39
Bruxism affects a meaningful minority of adults; studies typically report higher rates in younger and middle-aged adults than in older groups.
In the 30–39 age range, many experience either occasional or chronic bruxism tied to life stressors and sleep issues common in this decade.
Nighttime bruxism can be underreported because individuals are unaware of nocturnal activity.
Dentists usually detect it by examining wear patterns and asking targeted questions during routine visits.
Because prevalence varies by population and diagnostic method, individual risk depends on your stress load, sleep quality, medication use, and dental health.
If you fall into one or more higher-risk categories, expect a greater likelihood of persistent grinding that needs proactive management.
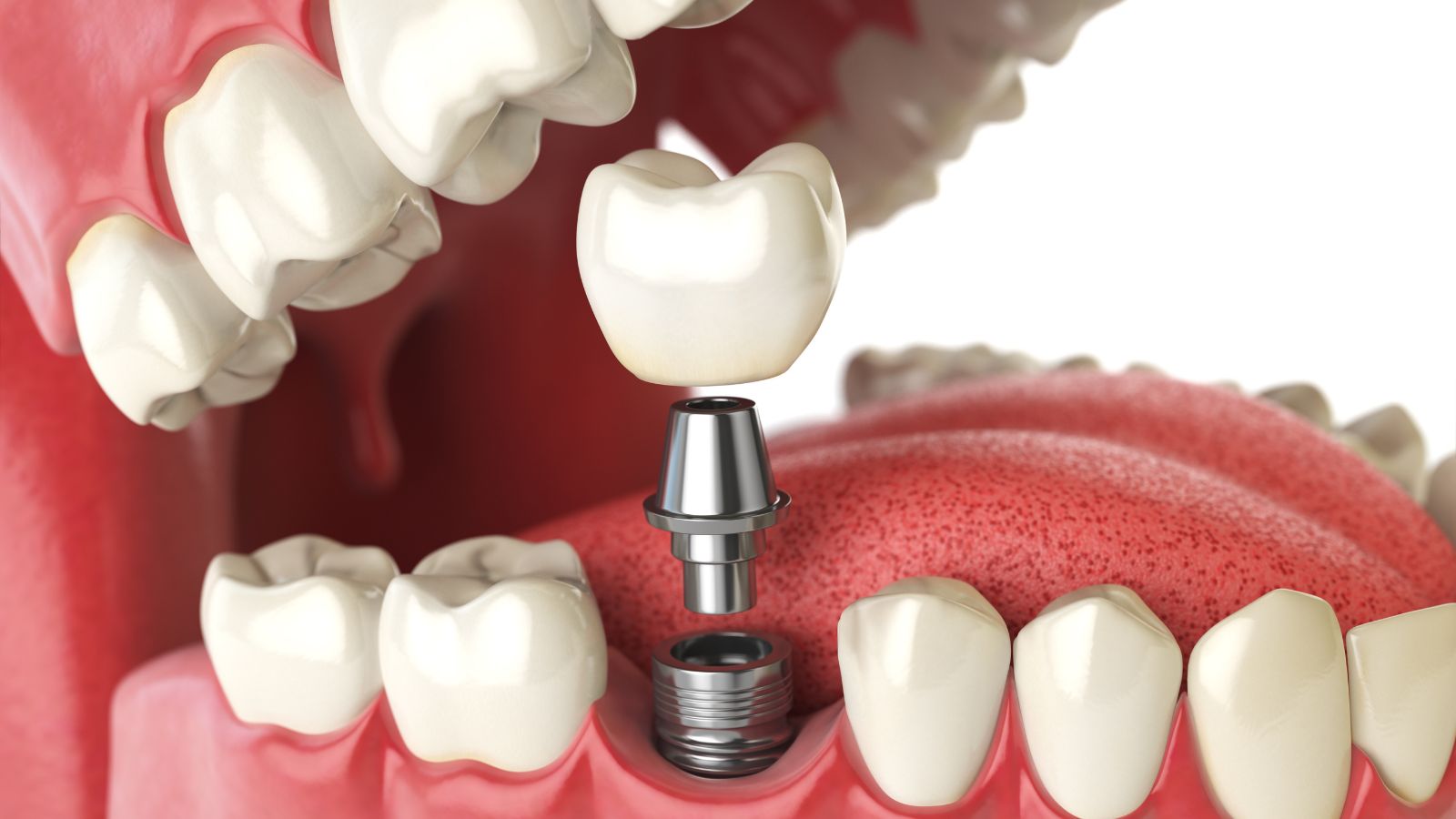
How Chronic Grinding Leads to Tooth Loss
Chronic grinding applies repeated, high-force pressure to teeth and the supporting structures. Over months and years this force wears enamel, damages gums and bone, and creates fractures that undermine tooth stability.
Wear and Damage to Tooth Enamel
When you grind, contact forces concentrate on small areas of enamel. Enamel thins and flattens first on biting surfaces and the edges of front teeth, increasing sensitivity and making teeth more prone to cavities.
As enamel wears away, dentin becomes exposed. Dentin is softer and wears faster, which accelerates loss of tooth height and alters your bite. Changes in bite can shift chewing forces to other teeth, creating a cycle of accelerated wear.
You may notice shorter teeth, flattened cusps, or visible chips. Restorations such as fillings and crowns can fail sooner because grinding repeatedly stresses the materials, leading to gaps, recurrent decay, or the need for replacement.
Gum Recession and Bone Loss
Grinding transfers excessive force to the periodontal ligament and the bone that supports each tooth. Over time these tissues respond by resorbing—gum tissue pulls back and alveolar bone can shrink.
Receding gums expose more root surface, which lacks protective enamel and is more vulnerable to decay and abrasion. Exposed roots also reduce the effective support for the tooth, making it more mobile under load.
If bone loss progresses, your dentist may detect increased tooth mobility or deeper periodontal pockets. Once significant bone support is lost, tooth extraction becomes more likely because the tooth can no longer withstand normal chewing forces.
Stress Fractures and Tooth Instability
Repetitive grinding creates microfractures in enamel and into dentin. These hairline cracks grow over time and can propagate beneath fillings or crowns, eventually splitting a tooth.
A cracked tooth may present as intermittent pain on biting or temperature sensitivity. Untreated cracks allow bacteria to invade the pulp, often requiring root canal therapy or extraction if infection or structural collapse occurs.
As fractures and supporting bone loss accumulate, your teeth lose mechanical stability. Mobility, shifting teeth, and complete separation of fractured segments can follow, leaving extraction or advanced prosthetic work as the only options to restore function.
Long-Term Health Risks of Untreated Bruxism
If you leave grinding untreated, expect progressive damage to tooth structure, dental work, and the tissues supporting your teeth. Each of the following risks accelerates tooth loss if you don’t address bruxism early.
Increased Risk of Tooth Decay
Grinding wears tooth enamel away, exposing the softer dentin beneath. Once dentin becomes exposed, sensitivity to hot, cold, and sweet foods increases and bacteria gain easier access to deeper tooth layers.
You also develop microcracks and craze lines from repeated stress. Those tiny defects trap plaque and are harder to clean, which raises your chance of cavities even if you brush regularly.
If decay reaches the pulp, you face root canal treatment or extraction. Preventing enamel loss with a night guard and treating early decay reduces this pathway to tooth loss.
Impact on Dental Restorations
Bruxism applies high, repetitive forces that shorten the lifespan of fillings, crowns, veneers, and implants. Composite fillings and porcelain crowns can chip, fracture, or debond under persistent grinding.
You may need frequent repairs or full replacement of restorations, which increases cost and reduces available tooth structure for future work. Implants and bridges also suffer: repeated overload can cause screw loosening, crown fracture, or bone loss around the implant.
Your dentist can adapt restorations (stronger materials, occlusal adjustments) and provide protective appliances, but untreated grinding steadily undermines even well-made dental work.
Potential for Advanced Periodontal Disease
Forceful clenching transmits abnormal pressure to the gums and the bone that supports your teeth. That pressure can accelerate loss of bone height around teeth, especially where gum disease already exists.
Grinding worsens gum recession and causes increased tooth mobility by stretching periodontal ligaments. Mobile teeth create deepening pockets that harbor bacteria and make professional cleaning less effective.
Combined with plaque-driven inflammation, the mechanical damage from bruxism raises the likelihood that periodontitis will progress to stages requiring tooth extractions. Treating both bruxism and periodontal disease together limits long-term tooth loss risk.
Proactive Steps to Protect Your Teeth
Act now to reduce forces on your teeth, manage contributing habits, and use dental treatments that prevent wear and loss. Practical changes at home and timely professional care together lower the risk that grinding in your 30s causes tooth fractures, recession, or eventual tooth loss.
Lifestyle Modifications and Stress Management
Identify when you clench or grind: during the day, at work, or when you sleep. Track triggers like caffeine, late-night screen time, or arguments and reduce them incrementally.
Use specific techniques to interrupt daytime grinding. Set phone reminders to relax your jaw, keep your teeth slightly apart, and swallow or reposition your tongue. Practice short, frequent jaw-relaxation exercises: open slowly, hold 5 seconds, then close gently.
Change habits that increase muscle tension. Cut back on caffeine and alcohol, stop smoking, and avoid chewing gum or hard candies. Aim for 7–8 hours of sleep and a winding-down routine—dim lights, limit screens 60 minutes before bed—to reduce nighttime clenching.
Add stress-reduction tools that fit your routine. Try 10-minute breathing breaks, progressive muscle relaxation, or guided meditation apps. If anxiety persists, seek cognitive-behavioral therapy or counseling to address underlying causes of bruxism.
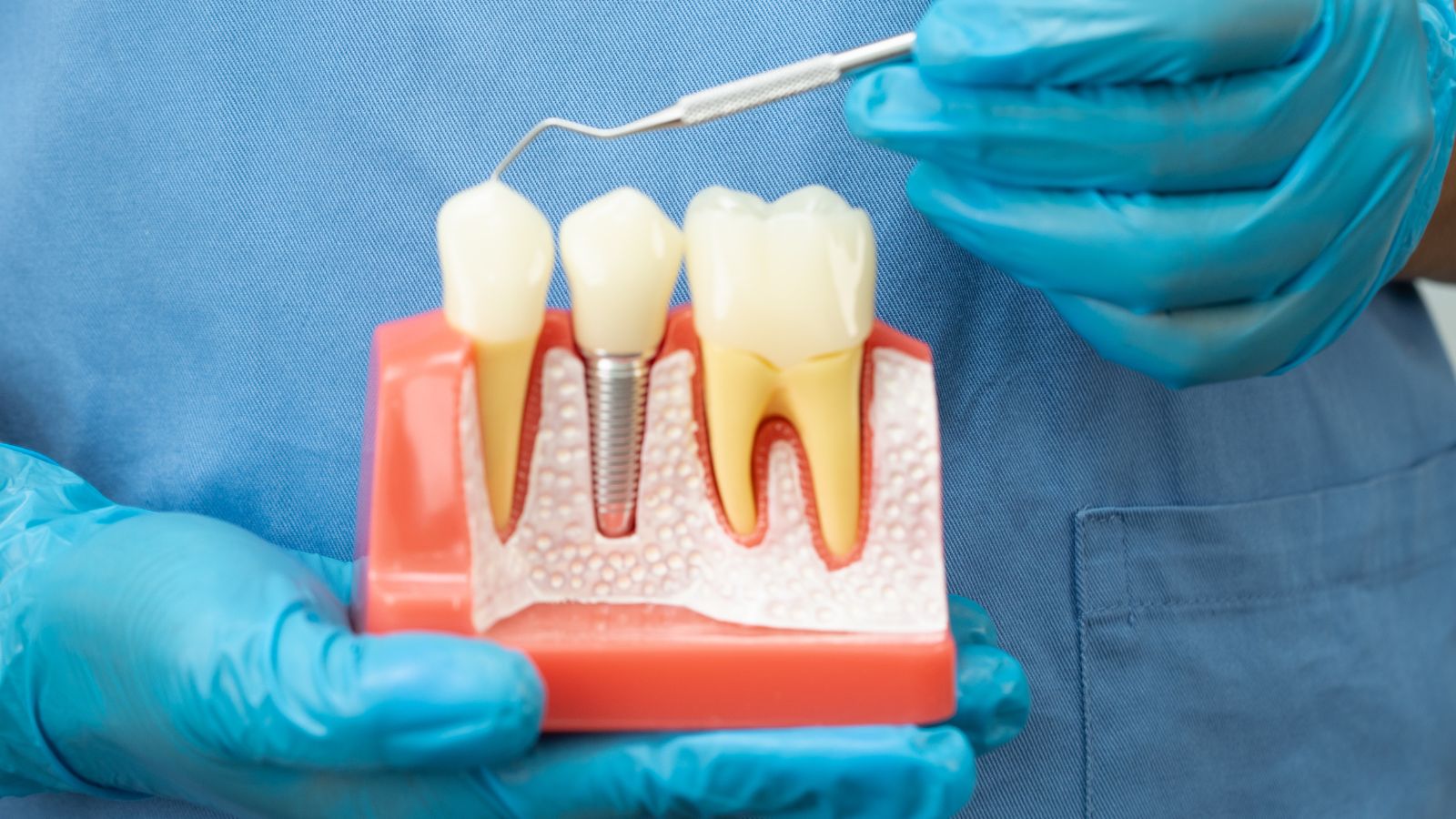
Professional Dental Interventions
Schedule a dental exam focused on wear patterns, tooth mobility, and jaw tenderness. Your dentist can document damage and recommend next steps before irreversible loss occurs.
Ask about a custom occlusal guard (night guard). A well-fitting appliance made from firm acrylic protects enamel, redistributes forces, and often reduces muscle activity during sleep. Bring concerns about comfort—adjustments improve compliance.
Consider bite equilibration or restorative work when uneven contacts drive grinding. Minimal reshaping of tooth surfaces or composite buildups can stop high-pressure contacts that initiate wear. For severe muscle pain, your dentist may coordinate with a physician about short-term muscle relaxants or referral to a TMJ specialist.
If sleep apnea is suspected, request a sleep study referral. Treating obstructive sleep apnea with CPAP or an oral appliance often reduces nighttime bruxism and protects teeth.
Benefits of Early Diagnosis and Prevention
Early detection preserves tooth structure and expands your treatment options. Minor enamel fractures or localized wear can be restored with bonding or conservative crowns, preventing more invasive procedures later.
Preventive measures lower long-term costs and complications. A custom night guard plus small habit changes often halts progression; waiting until teeth fracture may require root canals, crowns, or extraction and implants.
Diagnosis also lets you monitor progression objectively. Regular photos, bite records, and periodic radiographs let your dental team intervene at predictable stages rather than react to sudden tooth failure.