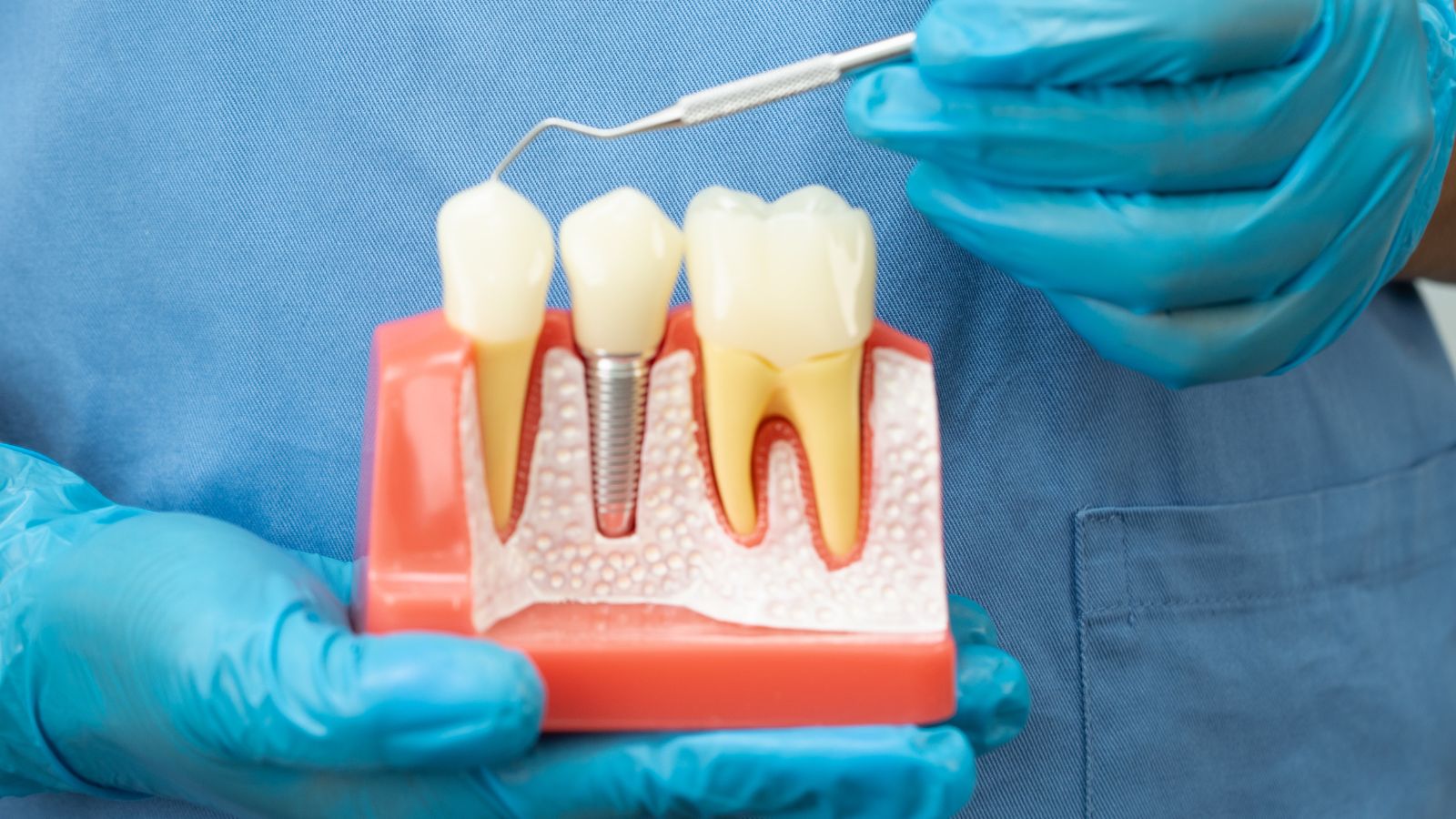
You likely want a quick, practical answer: if you’re in your 30s and lost a tooth in an accident, timing depends on injury severity, bone health, and whether any growth or infection needs to settle—but many adults can proceed with implants once the site is stable and any necessary bone grafting or soft-tissue healing is completed. If the area is infection-free and has adequate bone, your dentist can often place an implant within weeks to a few months; if not, expect additional healing or grafting that delays placement by several months.
This article will walk you through why timing matters, what medical and lifestyle factors to consider, the preparatory steps your dental team may recommend, and what recovery and long-term outcomes typically look like for people in their 30s.
You’ll get clear guidance to help plan realistic expectations, avoid unnecessary delays, and make informed decisions with your dentist, especially if you are exploring full arch dental implants in New Orleans as part of your long-term treatment options.
Table of Contents
ToggleWhy Timing Matters for Dental Implants After an Accident
Prompt action can preserve bone, reduce the need for grafting, and limit soft-tissue damage. Delays can increase complexity, cost, and the number of procedures you need.
Impact of Immediate Dental Care
If you seek dental care within days after the accident, clinicians can assess bone fractures, tooth viability, and soft-tissue injury while inflammation is low. That assessment lets your dentist or oral surgeon decide whether an immediate implant, tooth replantation, or temporary stabilization is appropriate.
Immediate treatment can preserve the socket and minimize bone resorption. When the implant or socket preservation measures occur quickly, you often avoid more invasive grafting later. You also reduce the risk of adjacent teeth shifting and changing bite relationships.
Immediate care also controls infection risk and manages soft-tissue lacerations that affect later esthetics. Prompt antibiotics, debridement, and suture placement improve healing and the long-term appearance of the implant site.
Risks of Delaying Implant Placement
Waiting months to replace a lost tooth after trauma often leads to progressive jawbone loss at the extraction site. Within the first year you can lose a significant portion of ridge height and width, which may force a bone graft before an implant.
Delay increases the chance of needing multiple surgeries: grafting, ridge augmentation, or sinus lift (in the upper back jaw). Each added procedure lengthens treatment time and raises cost and complication risk. You may also face compromised esthetics if the gum contour and papillae recede.
Additionally, untreated infection or an unstable occlusion after trauma can damage surrounding teeth and complicate implant planning. Longer waits can require orthodontic alignment or removable prostheses while you prepare the site for a reliable implant.
Optimal Healing Windows
Clinicians typically consider three timing strategies: immediate (at or right after extraction), early (weeks to a few months), and delayed (several months). Immediate placement suits sites with minimal infection, sufficient bone, and intact soft tissue. It helps preserve bone and shortens overall treatment time.
Early placement—after soft-tissue healing but before major bone loss—balances infection control with reduced resorption risk. Delayed placement allows complete healing after severe trauma or infection, but it often requires augmentation to rebuild lost bone and gum tissue.
Your dentist will evaluate factors such as socket integrity, infection status, amount of remaining bone, and overall health to pick the best window. Discuss timelines, likely need for grafting, and interim options (temporary crowns or removable prostheses) so you can plan function and appearance during healing.
Key Factors 30-Somethings Should Consider
You’ll weigh oral condition, jaw bone strength, medical background, and daily habits when deciding timing and type of implant. Each factor affects whether you can proceed immediately, need preparatory care, or should consider alternatives.
Assessing Oral Health After Trauma
Have your dentist evaluate injured teeth, surrounding gums, and soft tissue within days of the accident. Active infection, extensive gum recession, or unresolved root fractures increase the risk of implant failure and usually require treatment—root canals, extractions, or periodontal therapy—before implant placement.
Expect detailed imaging: periapical X-rays and a CBCT scan to check root remnants, fracture lines, and the exact position of adjacent teeth. Your clinician will look for healthy gum attachment and absence of pus or chronic inflammation; if present, they’ll treat it first and delay implant surgery until tissues are stable.
Maintain daily brushing with a soft brush and saltwater rinses as directed to control bacterial load while you wait. Timely management of soft-tissue injuries reduces scarring and improves the chance of predictable implant outcomes.
Bone Density and Age-Related Changes
Bone volume in the jaw determines whether an implant can be placed immediately or requires grafting. Trauma can cause localized bone loss; you’ll need a CBCT scan to measure ridge width and height and to map vital structures like the sinus or nerve canal.
At 30-something, you typically have good baseline bone quality, but the specific injury may create defects that require bone grafts or guided bone regeneration. If grafting is needed, plan for an additional healing window of 3–6 months before implant placement in many cases.
Your clinician may recommend immediate implant placement when bone and soft tissue are sufficient; otherwise, staged reconstruction improves long-term stability. Understand the timeline and graft material choices (autograft, allograft, xenograft, or synthetic) before consenting.
Medical History and Medications
Share a complete medical history including chronic conditions, prior surgeries, and current medications with your dental team. Conditions such as uncontrolled diabetes, autoimmune disorders, or therapies that affect bone turnover (bisphosphonates, denosumab) change implant candidacy and timing.
Smoking and vaping reduce blood flow and delay healing; quitting at least several weeks before surgery and maintaining abstinence during osseointegration improves success rates. Also report recent or planned radiotherapy to the head/neck and any anticoagulant or immunosuppressive medications—your dentist will coordinate with your physician on perioperative management.
If you take medications that influence bone metabolism, expect specialist input and possibly altered timelines. Clear communication prevents surprises and reduces risk during surgery and healing.
Lifestyle and Recovery Expectations
Plan for a recovery period that may include limited chewing, a soft-food diet, and time off work if your job is physically demanding. Immediate implant placement often involves less total time off but can carry higher short-term sensitivity when tissues are compromised.
Be prepared for multiple appointments: initial imaging, any preparatory procedures (extraction, grafting), implant placement, and prosthetic phases. Daily oral hygiene and compliance with follow-up visits directly affect osseointegration and long-term success.
Consider financial and scheduling realities now. Implants after trauma often require staged care and specialist visits (oral surgeon, periodontist, prosthodontist); factor costs, insurance limits, and time into your decision so you can commit to the full treatment plan.
Steps to Take Before Getting Dental Implants
You’ll need to confirm medical and dental fitness, obtain detailed imaging, and agree on a step-by-step treatment plan that fits your recovery time and work/life schedule.
Consulting with Dental Professionals
Start with a consultation that includes both a restorative dentist (or prosthodontist) and an oral surgeon if possible. Bring your medical history, any accident reports, and a list of current medications—blood thinners, bisphosphonates, and immunosuppressants can change timing or require coordination with your physician.
Discuss anesthesia options (local with sedation vs. general), expected number of visits, short- and long-term costs, and whether grafting or extractions will be needed first.
Ask for experience treating trauma-related tooth loss and request before/after photos of similar cases. Get clear instructions on preoperative fasting, smoking cessation, and pain-management plans so you can prepare work leave and support at home.
Diagnostic Imaging and Evaluations
Expect periapical and panoramic X-rays plus a CBCT 3D scan to assess bone volume, sinus position, and proximity to nerves. These images determine whether your jaw has sufficient height, width, and density for implant placement or if a bone graft, sinus lift, or nerve repositioning is required.
Your dentist will also evaluate adjacent teeth, occlusion (how your bite meets), and soft-tissue health. Laboratory tests or clearance from your primary care doctor may be requested if you have systemic conditions.
Keep copies of all scans and reports; they help if you seek a second opinion or need coordination with a specialist.
Treatment Planning and Timeline
Your provider will map a staged timeline: extractions and healing, grafting (if needed) and integration, implant placement, osseointegration (usually 3–6 months), and crown placement. Trauma cases often add healing time for bone grafts or soft-tissue repair.
Request a written plan with dates or ranges, number of appointments, estimated healing windows, contingency steps (e.g., graft failure), and cost breakdowns for each stage.
Confirm temporary tooth options during healing, follow-up visit frequency, and criteria your team will use to move from one stage to the next so you can plan work, travel, and activity restrictions.
Post-Implant Recovery and Long-Term Outcomes
You will follow a predictable healing sequence, manage common discomfort with targeted measures, and support long-term success through hygiene, lifestyle choices, and regular checkups.
Expected Healing Timeline
Expect the first 48–72 hours to show the most swelling and bleeding; use ice packs for 15 minutes on/off and avoid strenuous activity.
Sutures (if used) often come out or dissolve within 7–14 days; call your clinician if you see heavy bleeding, rising pain, or spreading redness.
Osseointegration — the bone fusing to the implant — typically takes 3–6 months depending on bone quality and whether you had grafting.
If your surgeon places a temporary crown, avoid chewing on that side until the final restoration is placed. Final prosthesis timing depends on implant stability (measured as torque or ISQ).
Follow prescribed antibiotics or antiseptic rinses exactly. Missed meds or early loading can increase failure risk.
Managing Discomfort and Complications
Use recommended analgesics (NSAIDs or acetaminophen) and follow dose limits; avoid aspirin if your surgeon advised against it.
Cold packs help first 48 hours; warm compresses reduce muscle tension after 72 hours.
Watch for signs of infection: persistent swelling beyond 5–7 days, fever, or increasing pain.
Contact your dentist promptly for loosening, pus, or numbness that doesn’t improve. Early intervention (cleaning, antibiotics, sometimes implant removal) prevents larger problems.
Be aware of nerve injury or sinus issues after trauma-related implants.
If you experience altered sensation or sinus congestion, report it immediately so your surgeon can assess with imaging and choose appropriate treatment.
Ensuring Implant Longevity
Practice daily oral hygiene: brush twice with a soft brush and floss or use interdental brushes around the implant crown.
Consider a low-abrasive toothpaste and a water flosser if dexterity is limited.
Schedule professional maintenance every 3–6 months initially, then at least annually; the clinician will check soft tissue, probe depths, and radiographs for bone levels.
Manage risk factors: stop smoking, control diabetes (HbA1c ideally <7%), and address bruxism with a nightguard to reduce overload.
Keep records of implant brand, size, and placement date; this information speeds treatment if complications occur.
Report any changes—movement, pain, or gum recession—early to preserve bone and avoid complex revision surgery.