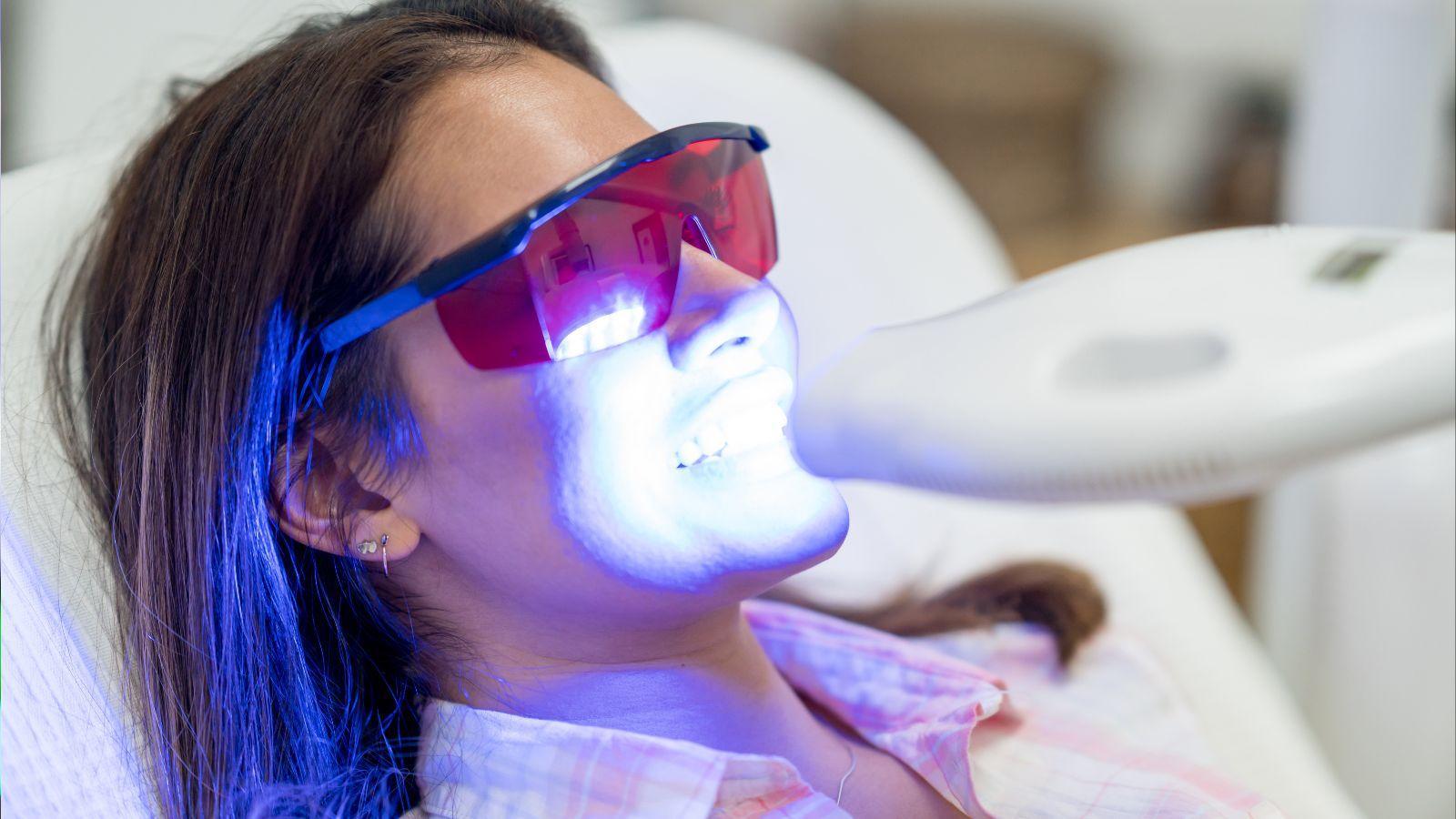
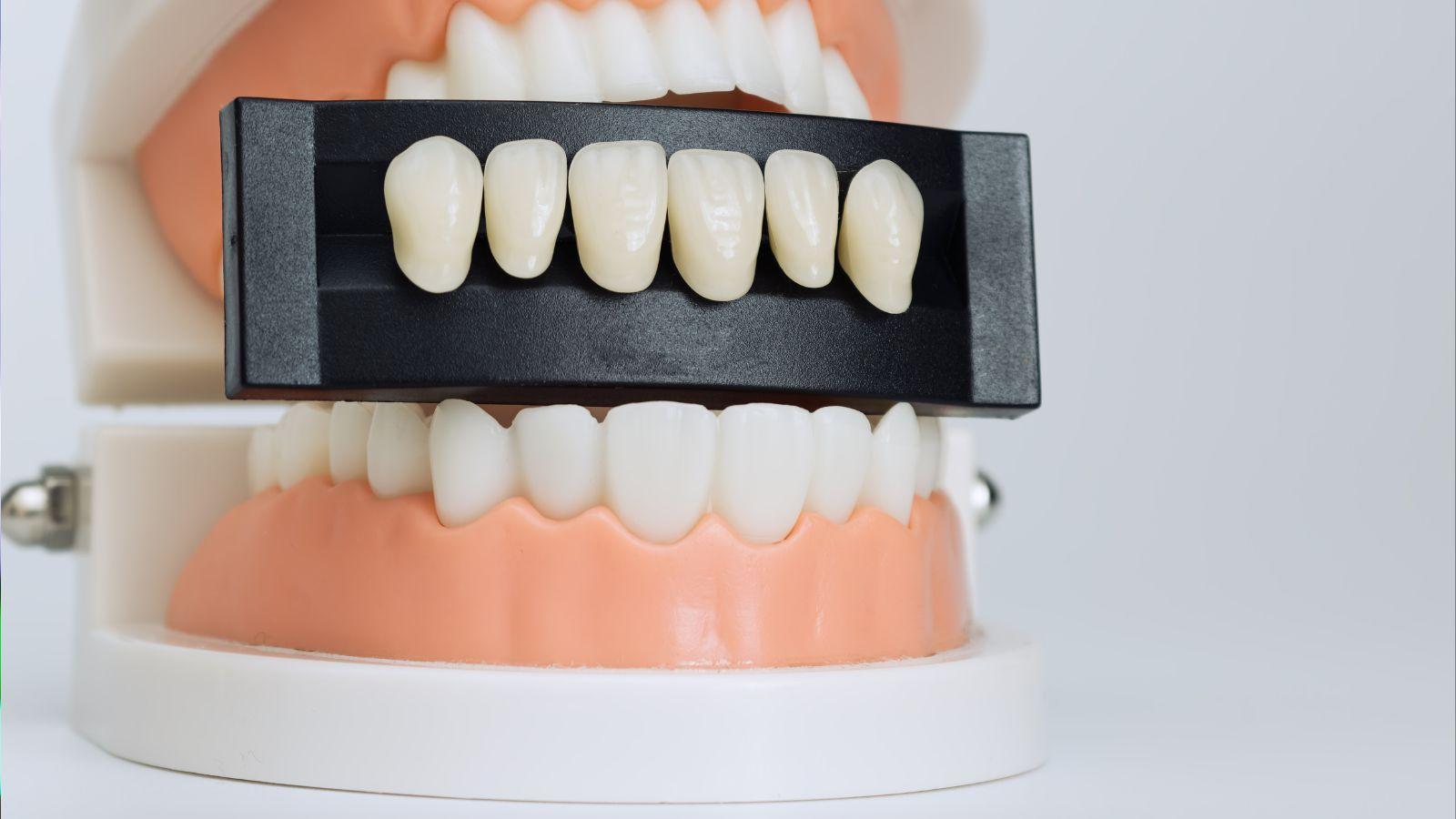
You want a level of clean that removes hidden grime, disinfects high-touch spots, and reaches places you usually skip. A deep cleaning is a thorough, one-time or occasional clean that tackles hard-to-reach areas, built-up dirt, and germs, while a regular clean keeps surfaces tidy with routine tasks like dusting, vacuuming, and wiping — just like a dentist in Florida takes a thorough approach to deep cleaning versus routine checkups.
Knowing this helps you pick the right job for your schedule, health needs, or an upcoming event. The next sections will show the core steps of a deep clean, what routine cleaning covers, when each approach fits best, and how to keep your space fresh after a deep clean.
Table of Contents
ToggleCore Steps of Deep Cleaning
You will focus on removing buildup, treating infected areas, and protecting tissues afterward. The steps below explain what each part does and what you should expect during treatment.
Scaling and Root Planing
Scaling removes hardened deposits from tooth surfaces and below the gumline. Your hygienist or dentist uses manual scalers and ultrasonic tools to loosen and lift tartar. Expect scraping sensations and some pressure; local anesthesia can numb the area for comfort.
Root planing smooths the root surfaces after scaling. Smoother roots help gums reattach and reduce places where bacteria hide. Your provider will gently file rough spots until the root feels clean and even.
After these steps, bleeding and mild soreness are common for a few days. You may get post-care instructions like gentle brushing, saltwater rinses, and avoiding hard foods while tissues heal.
Plaque and Tartar Removal Below the Gumline
Plaque forms from bacteria and food particles; if not removed it hardens into tartar (calculus) that bonds to teeth. Below the gumline, tartar sits against the root and causes inflammation. You need targeted tools to reach these tight spaces.
Providers examine pocket depth with a probe to decide how deep to treat. Pockets over 4 mm often require more intensive cleaning. They will work methodically, quadrant by quadrant, to clear deposits and reduce pocket depth.
Removing subgingival tartar lowers bacterial load and slows disease. You might feel sensitivity when roots are exposed; this usually eases with proper home care and any recommended desensitizing products.
Antibacterial Treatments
After physical cleaning, antibacterial treatments reduce remaining bacteria and help healing. Your clinician may apply a local antibiotic gel or place small antibiotic chips into deep pockets. These deliver medication directly where you need it.
In some cases they rinse with an antimicrobial solution or prescribe a short course of oral antibiotics. You must follow dosing instructions exactly to avoid resistance and ensure effectiveness.
Antibacterial therapy helps control infection and supports gum reattachment. It is not a substitute for good brushing and flossing; you must keep up daily care to prevent recurrence.
Routine Cleaning Procedures
These routine steps keep your mouth healthy between deeper treatments. They focus on removing surface stains, clearing soft deposits above the gumline, and strengthening enamel.
Tooth Polishing
Tooth polishing removes surface stains and smooths enamel after scaling or cleaning. Your dental hygienist uses a rotating rubber cup or brush with a gritty prophylaxis paste. The paste contains mild abrasives and a polishing agent that lifts coffee, tea, and tobacco stains without harming healthy enamel.
Polishing also makes teeth feel smoother by evening out tiny rough spots where plaque can cling. Expect brief bursts of polishing on each tooth, usually lasting a few seconds per area. If you have sensitive teeth, your hygienist can use a low-abrasive paste or skip polishing on tender spots.
You may notice a brighter appearance and a clean, slick feel. Polishing does not replace brushing at home. Keep up daily brushing and flossing to prevent stains from returning quickly.
Plaque and Tartar Removal Above the Gumline
Plaque removal uses manual or powered scalers to scrape soft bacterial film from tooth surfaces. Your hygienist targets the areas where plaque builds up fastest: along the gumline, between teeth, and around restorations.
Tartar (calculus) forms when plaque hardens. The hygienist removes tartar above the gumline with stainless steel curettes or ultrasonic scalers that vibrate and spray water to break off deposits. This prevents gum irritation and helps keep gums firm and pink.
You may feel scraping or mild vibration, and your mouth might be sensitive afterward. The process lowers your risk of gingivitis by reducing bacteria that cause inflammation. Regular visits every 3–6 months keep buildup under control.
Fluoride Application
Fluoride application strengthens enamel and helps prevent cavities after cleaning. Your hygienist may use a gel, foam, or varnish applied with a brush, tray, or swab. Varnish dries quickly and sticks to teeth for prolonged benefit.
The treatment takes a few minutes. You should avoid eating, drinking, or rinsing for 30–60 minutes after varnish so fluoride can absorb. For gels or foams, you might bite on a tray for a short time.
Fluoride suits most patients but the hygienist will adjust concentration for children or those with special needs. Regular topical fluoride adds protection between cleanings, especially if you have past decay or enamel wear.
Key Differences and Appropriate Uses
Deep cleaning targets hidden dirt, buildup, and high-touch germ hotspots. Regular cleaning focuses on visible dirt, daily hygiene, and keeping spaces tidy and functional.
Ideal Candidates
You should choose a deep clean if your space shows signs of long-term buildup, like grimy grout, greasy kitchen hoods, or dusty vents. Move-in or move-out situations, post-construction sites, and properties that haven’t had routine maintenance for months also need deep cleaning. Businesses with high foot traffic, healthcare settings, or restaurants should schedule deep cleans to reduce disease risk and meet regulatory standards.
Regular cleaning fits homes and offices with steady upkeep. You need it if you want dusting, vacuuming, trash removal, surface wiping, and bathroom sanitizing done weekly or biweekly. Use regular cleaning to maintain appearances and prevent the buildup that would later require a deep clean.
Objectives of Each Cleaning Type
Deep cleaning aims to remove embedded dirt, mold, grease, and allergens. It includes tasks like scrubbing grout, cleaning inside appliances, descaling fixtures, steam-cleaning carpets, and cleaning HVAC vents. The goal is restorative: restore surfaces to near-new condition and address health risks not solved by routine cleaning.
Regular cleaning aims to control surface dirt and germs, keep spaces organized, and support daily operations. Tasks include wiping counters, emptying bins, sweeping and mopping floors, cleaning mirrors, and disinfecting toilets and sinks. The goal is maintenance: reduce visible dirt and lower immediate infection risk.
Treatment Frequency
Plan deep cleaning on a schedule based on use and condition: every 6–12 months for homes, quarterly for commercial kitchens, and monthly for high-risk healthcare areas. Trigger deep cleans after renovations, infestations, or when allergies and odors persist despite regular cleaning.
Use regular cleaning more frequently: daily or several times per week for busy commercial spaces, weekly for most households, and biweekly for low-use areas. Adjust frequency based on pets, children, allergy sufferers, and foot traffic to prevent the need for unscheduled deep cleaning.
Potential Outcomes and Aftercare
You may feel sore or tender after a deep cleaning. This is normal and usually eases in a few days. Over-the-counter pain relievers and cold packs can help.
Your gums might bleed for a short time and look puffy. Good oral hygiene speeds healing. Brush gently, floss carefully, and avoid hard or crunchy foods for a few days.
You can expect increased tooth sensitivity, especially to hot or cold. Sensitivity often improves over weeks. Your dentist may recommend desensitizing toothpaste or fluoride treatments to reduce discomfort.
Your mouth needs follow-up care to stay healthy. You will likely need more frequent cleanings—often every three months—instead of the usual six. These maintenance visits help prevent the gum disease from returning.
Watch for signs that need prompt care: persistent pain, swelling that worsens, or pus around the gums. Contact your dentist if you have these symptoms, or if bleeding does not slow after a day or two.
Simple aftercare tips:
- Rinse with warm salt water 2–3 times daily to soothe tissues.
- Avoid smoking and alcohol for at least 48 hours to help healing.
- Take antibiotics or other meds only if your dentist prescribes them.
Keep a record of your symptoms and share them at follow-up visits. This helps your dental team adjust treatment and protect your long-term oral health.