You might not expect tooth loss to become a real risk in your 30s, but gum disease quietly damages gum and bone long before you notice major symptoms. If you act now—by recognizing early signs, improving daily care, and seeing a family dentist in Champaign IL —you can prevent most tooth loss caused by periodontitis.
Many people in their 30s dismiss bleeding gums or bad breath as minor annoyances, yet those are early warnings that the infection is taking hold beneath the gumline. This article explains what early gum disease looks like in your 30s, why it often goes unnoticed, and the practical prevention and treatment steps that actually protect your smile.
Table of Contents
ToggleUnderstanding Gum Disease in Your 30s
Gum disease in your 30s can progress without pain and quietly weaken the bone and tissues that hold your teeth. Early signs are often subtle, but timely care and specific habits can stop damage before tooth loss begins.
What Is Gum Disease?
Gum disease is an infection of the tissues that support your teeth—your gums, periodontal ligament, and jawbone. It begins when plaque, a sticky film of bacteria, builds up along the gumline and triggers inflammation.
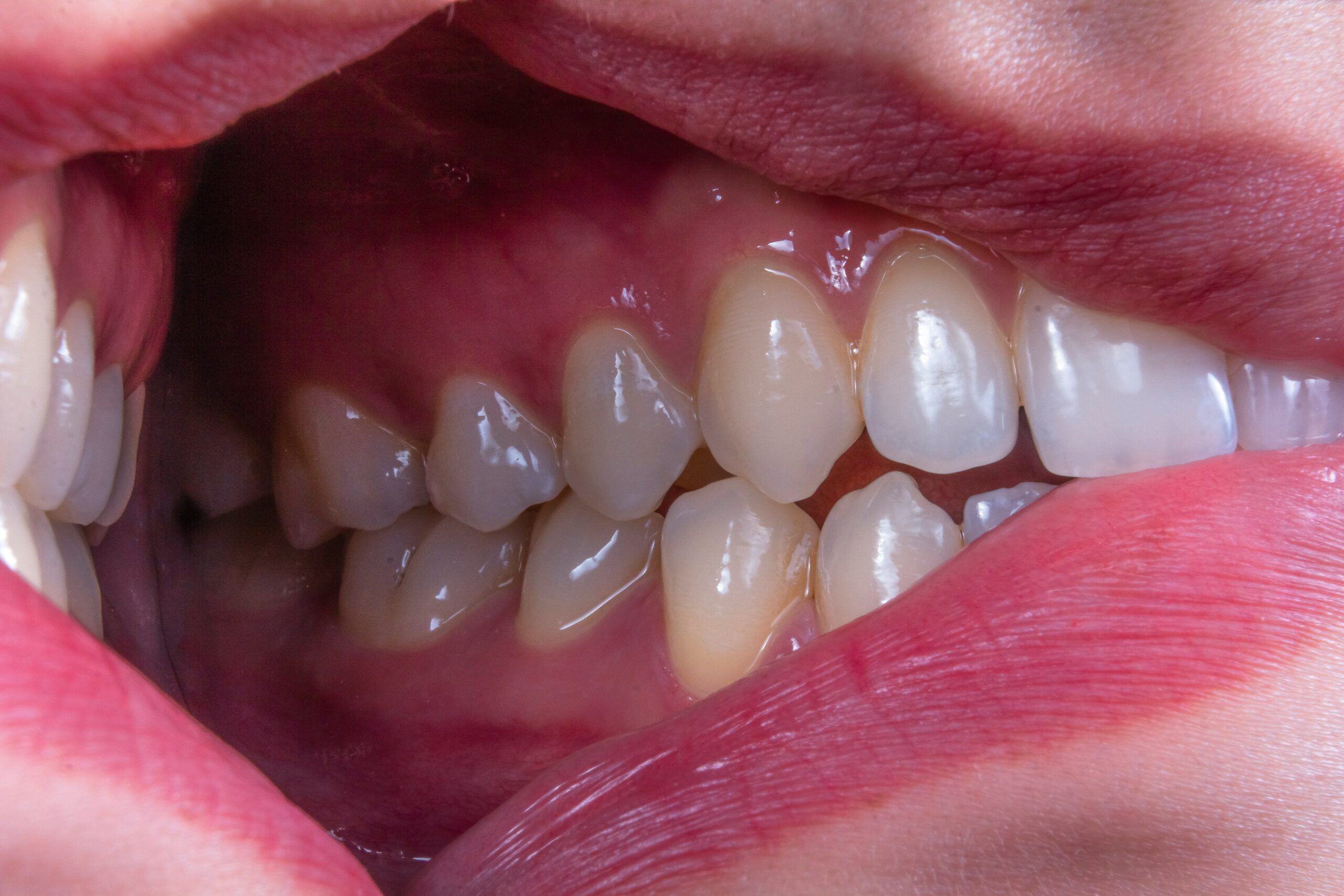
You’ll first notice signs like bleeding when you brush, persistent bad breath, or gums that look redder or swollen than usual. If untreated, inflammation deepens into pockets between teeth and gums where bacteria multiply and bone can be lost. Treatment ranges from improved home care to professional cleanings and, in advanced cases, scaling, root planing, or periodontal surgery.
Why It Often Goes Undetected
Many people in their 30s ignore early gum disease because it’s usually painless. Bleeding when brushing can seem minor, and bad breath may be blamed on diet or stress instead of infection.
Symptoms can be intermittent or dismissed as normal. Routine dental checkups may be skipped, especially if you don’t feel pain. Also, early bone loss doesn’t show on the surface, so only measurements, X-rays, or probing by a dental professional reveal the true extent of damage.
Types and Stages of Gum Disease
Gum disease progresses along a continuum with clear clinical stages:
- Gingivitis: Reversible inflammation confined to gums. Symptoms: bleeding, redness, swelling. You can reverse it with improved brushing, flossing, and professional cleaning.
- Early periodontitis: Inflammation extends below the gumline; small pockets form and slight bone loss may appear on X-rays.
- Moderate to advanced periodontitis: Deeper pockets, significant bone loss, tooth mobility, and possible tooth loss.
Key risk factors that accelerate progression include smoking, uncontrolled diabetes, poor oral hygiene, and genetic susceptibility. Your dentist uses pocket probing, clinical attachment loss, and X-rays to stage disease and guide treatment.
Why Gum Disease in Your 30s Is a Silent Threat
Gum disease in your 30s often starts without pain but shows small, specific changes that predict faster damage. You may notice bleeding, persistent bad breath, or shifting teeth long before major problems appear.
Subtle Warning Signs to Watch For
Look for bleeding when you brush or floss, even if it seems minor. Bleeding indicates inflammation of the gums (gingivitis) that can progress; ignoring it lets bacteria move below the gumline.
Monitor for persistent bad breath that brushing and mints don’t fix. That odor often comes from bacterial biofilm and trapped food debris in deepening pockets around teeth.
Note changes in bite or loose-feeling teeth. Teeth that feel different when chewing signal loss of supporting bone and connective tissue. Also watch for receding gums and exposed tooth roots, which increase sensitivity and cavity risk.
How Early Gum Disease Leads to Tooth Loss
Gum disease begins with plaque that hardens into tartar, which you can’t remove at home. Tartar and bacteria cause inflammation that destroys the connective tissue attaching tooth to bone.
As pockets deepen, bacteria travel deeper and bone resorption accelerates. Over months to years, the bone level drops and teeth lose their foundation; mobility increases and extraction may become necessary.
Professional scaling and root planing can halt progression if done early. Once significant bone loss occurs, treatments like bone grafts or tooth replacement become more complex and costly.
Risks Unique to Adults in Their 30s
Busy schedules, young families, or career demands often reduce time for consistent oral care. Missed dental cleanings and rushed brushing raise your risk of undetected gum disease.
Lifestyle factors common in your 30s—smoking, weight gain, poor sleep, and stress—worsen inflammation and impair healing. Hormonal changes for some people can also increase gum sensitivity.
Genetics and past orthodontic work affect risk too. If you have a family history of periodontitis or crowded/overlapping teeth, you need more frequent monitoring and targeted preventive care.
Prevention and Effective Treatment Options
You can prevent most gum disease and stop early damage with specific daily habits, targeted in-office treatments, and regular professional follow-up. Focus on plaque control, reduce risk factors like smoking, and get prompt periodontal care when pocketing or bleeding appears.
Innovative Dental Care Strategies
Use an electric toothbrush with a soft brush head and a 2-minute timer to remove plaque more consistently than a manual brush. Replace the head every 3 months or sooner if bristles splay.
Floss once daily using floss or interdental brushes sized to the gaps between your teeth; interdental brushes often clean better when spaces are wider. Add a fluoride toothpaste and consider a 0.12–0.2% chlorhexidine rinse short-term only for persistent bleeding after discussing it with your dentist.
Consider adjuncts like a water flosser for hard-to-reach spots and daily antimicrobial mouthwashes if you have high plaque scores. If you have dry mouth from medications, ask about saliva substitutes or prescription options to reduce bacterial buildup.
Professional Interventions and Therapies
Schedule a professional cleaning (prophylaxis) every 3–6 months based on your risk. Hygienists remove calculus that brushing can’t, which reduces pocket inflammation and bacterial load.
If pockets exceed 4 mm or bleeding persists, your dentist will perform scaling and root planing (deep cleaning) to remove subgingival plaque and smooth root surfaces. This procedure often requires local anesthesia and multiple visits.
For advanced cases or complex anatomy, your dentist may refer you to a periodontist for surgical options such as flap surgery, regenerative procedures (bone or tissue grafts), or pocket reduction. Antibiotics—topical or systemic—may be used adjunctively when indicated by an infection or systemic risk factors.
Reversing Early-Stage Gum Disease
When you catch gingivitis early, you can reverse it with improved home care combined with a professional cleaning. Start by doubling down on brushing frequency and technique; remove plaque at the gumline and use interdental cleaning daily.
Your hygienist can provide tailored instruction and measure pocket depths to track improvement every 4–6 weeks after initial treatment. Short courses of prescription antimicrobial mouthwash or a localized antibiotic gel placed into pockets can accelerate healing when standard care alone is insufficient.
Monitor progress: reduced bleeding on probing, shrinking pocket depths, and healthier pink gum tissue indicate reversal. If these signs don’t appear within 6–8 weeks, expect further periodontal evaluation and possibly deeper treatments.
Long-Term Oral Health Maintenance
Set a personalized recall schedule—every 3, 4, or 6 months—based on your periodontal risk and treatment response. Stick to those visits to remove new calculus and reassess pocket depths.
Control systemic factors: quit smoking, manage diabetes tightly (A1c targets with your physician), and maintain a balanced diet high in vitamins C and D. Track medications that cause dry mouth and discuss alternatives with your prescriber.
Keep a simple home checklist: brush twice daily with an electric brush, floss or use interdental brushes once daily, use prescribed rinses as directed, and log any bleeding, loosening, or persistent bad breath to report at your next dental visit.